Red, itchy, irritated eyes are one of the most common reasons patients visit an eye doctor. While many people quickly assume they have “pink eye,” the reality is that not all conjunctivitis is the same. Understanding allergic vs infectious conjunctivitis is essential because the cause determines the correct treatment, and using the wrong approach can prolong symptoms or even make them worse.
Eye doctors rely on a combination of symptom patterns, medical history, and clinical examination to accurately tell these two conditions apart. In this article, we’ll explore how professionals diagnose allergic vs infectious conjunctivitis, what signs they look for, and why proper diagnosis matters for fast, safe relief.
Understanding Conjunctivitis and Why Diagnosis Matters
Conjunctivitis refers to inflammation of the conjunctiva, the thin membrane that covers the white part of the eye and lines the eyelids. While redness is common to all types, the underlying causes vary significantly. Eye doctors focus on identifying allergic vs infectious conjunctivitis early because treatment strategies differ and misdiagnosis can delay healing.
Allergic conjunctivitis is triggered by allergens like pollen, dust mites, pet dander, or mold. Infectious conjunctivitis, on the other hand, is caused by viruses or bacteria and can be highly contagious. Knowing which type you have helps prevent unnecessary medication use and limits the spread of infection. Because infectious conjunctivitis (viral or bacterial) can spread to others, differentiating it from non-contagious allergic conjunctivitis through clinical exam and symptom history is essential.
Key Symptom Differences Eye Doctors Look For
One of the first steps in diagnosing allergic vs infectious conjunctivitis is a detailed discussion of symptoms. While both conditions cause redness and irritation, the nature of the symptoms often provides valuable clues.
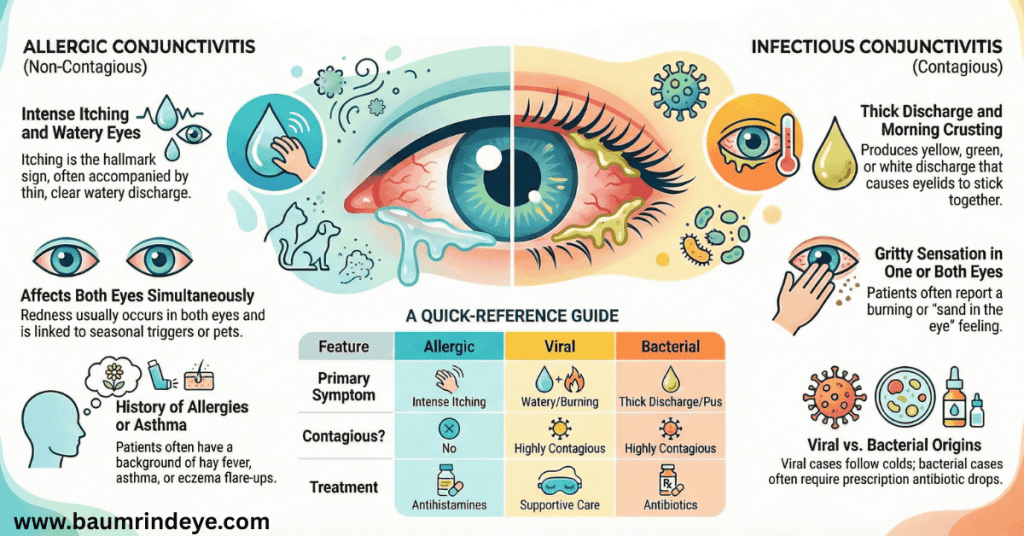
Symptoms Suggesting Allergic Conjunctivitis
- Intense itching (a hallmark sign)
- Watery discharge
- Redness in both eyes
- Seasonal or recurring symptoms
- History of allergies, asthma, or eczema
Symptoms Suggesting Infectious Conjunctivitis
- Thick discharge (yellow, green, or white)
- Crusting of the eyelids, especially in the morning
- Redness in one or both eyes
- Gritty or burning sensation
- Recent illness or exposure to someone with pink eye
These symptom patterns help eye doctors begin distinguishing allergic vs infectious conjunctivitis, even before the physical exam begins.
The Role of Medical History in Diagnosis
Medical history plays a major role in identifying allergic vs infectious conjunctivitis. Eye doctors ask targeted questions to uncover potential triggers or exposure risks, such as:
- Recent colds or respiratory infections
- Contact with someone who has pink eye
- Use of contact lenses
- Seasonal allergy flare-ups
- Environmental exposures (pets, pollen, dust)
A patient with chronic springtime eye itching and sneezing is more likely dealing with allergies, while sudden redness following a viral illness points toward an infection. These insights narrow down the diagnosis before any instruments are used. Baumrind Eye explains that allergic conjunctivitis causes red, watery, and itchy eyes when the conjunctiva becomes inflamed due to allergens like pollen, dust, mold, or pet dander.
Clinical Eye Examination Techniques
A thorough eye exam is essential when diagnosing allergic vs infectious conjunctivitis. Eye doctors use specialized tools like slit lamps to examine the surface of the eye, eyelids, and tear film in detail.
What Eye Doctors Look For:
- Discharge type: Watery discharge often suggests allergies or viral infection, while thick pus-like discharge suggests bacterial infection.
- Conjunctival appearance: Allergic conjunctivitis may show a swollen, pale conjunctiva, while infectious forms often appear intensely red.
- Eyelid involvement: Crusting and swelling may indicate infection.
- Corneal involvement: If the cornea is affected, further testing may be required.
These visual cues help confirm whether the condition is allergic or infectious and guide appropriate care.
When Lab Tests Are Needed
Most cases of conjunctivitis can be diagnosed clinically, but in severe, recurrent, or unclear cases, additional testing may be needed. Cultures or swabs are sometimes used when symptoms do not improve or when the diagnosis of allergic vs infectious conjunctivitis remains uncertain.
Testing is more common in suspected bacterial infections that are resistant to standard care or in patients with compromised immune systems.
Treatment Approaches Based on Diagnosis
Once eye doctors identify the cause, treatment can begin promptly. The correct approach depends entirely on whether the diagnosis leans toward allergies or infection.
For allergies, allergic conjunctivitis treatment focuses on reducing inflammation and blocking allergic reactions. This may include antihistamine drops, mast cell stabilizers, or lifestyle changes to reduce allergen exposure.
For infections, infectious conjunctivitis treatment depends on whether the cause is viral or bacterial. Bacterial cases may require prescription medication, while viral cases are usually managed with supportive care.
In some situations, doctors may recommend specific pink eye eye drops to relieve redness, irritation, and discomfort while the eye heals.
Viral vs Bacterial Pink Eye: A Closer Look
When evaluating allergic vs infectious conjunctivitis, doctors also determine whether infectious cases are viral or bacterial. Viral conjunctivitis often accompanies colds or flu and spreads easily, while bacterial conjunctivitis tends to produce thicker discharge.
Viral pink eye treatment typically involves symptom relief, artificial tears, and time, as antibiotics are not effective against viruses. Identifying the type helps avoid unnecessary medications and reduces antibiotic resistance.
Why Accurate Diagnosis Is So Important
Correctly distinguishing allergic vs infectious conjunctivitis protects both eye health and public health. Treating allergies with antibiotics offers no benefit, while missing an infectious cause can allow the condition to worsen or spread to others.
Accurate diagnosis ensures:
- Faster symptom relief
- Proper medication use
- Reduced risk of complications
- Prevention of unnecessary contagion
This precision is why professional evaluation is always recommended for persistent or severe eye symptoms.
Final Thoughts
Red, irritated eyes may look the same on the surface, but the cause matters greatly. Eye doctors use symptom patterns, medical history, and detailed exams to accurately diagnose allergic vs infectious conjunctivitis and provide targeted care. If your symptoms persist, worsen, or affect your vision, professional evaluation is the safest way to protect your eye health and recover quickly. Visit Baumrind Eye Care for expert treatment, personalized eye health solutions, and advanced care focused on clear vision and lasting comfort. Contact Baumrind Eye Care today to schedule appointments, ask questions, or get professional support for all your eye health concerns.
FAQs About Allergic and Infectious Conjunctivitis
How is allergic conjunctivitis treated?
Treatment typically includes antihistamine or anti-inflammatory eye drops, avoiding known allergens, and using cold compresses to relieve itching and swelling.
What is the best treatment for infectious conjunctivitis?
The best treatment depends on whether the infection is viral or bacterial. Bacterial cases may require prescription medication, while viral cases usually resolve with supportive care.
Do I need antibiotics for infectious conjunctivitis?
Antibiotics are only needed for bacterial infections. Viral conjunctivitis does not respond to antibiotics and usually clears on its own.
Can allergy eye drops help with pink eye?
Allergy eye drops can help if pink eye symptoms are caused by allergies, but they will not treat infectious conjunctivitis.
How can I prevent allergic conjunctivitis?
Prevention includes avoiding allergens, keeping windows closed during high pollen seasons, using air purifiers, and washing hands and face after outdoor exposure.






